In April 2023, a significant stride was made towards redefining the future of healthcare data management and interoperability with the unveiling of the HTI-1 Final Rule by the Office of the National Coordinator for Health Information Technology (ONC). This initiative, formally named “Health Data, Technology, and Interoperability: Certification Program Updates, Algorithm Transparency, and Information Sharing,” represents a pivotal evolution in healthcare technology, emphasizing enhanced data exchange and system interoperability. HTI-1, with its distinctive nomenclature, underscores a fresh, forward-looking approach to healthcare technology, positioning itself as the first of its kind in a series of progressive regulatory frameworks.
HTI-1 Framework Overview
The HTI 1 Final Rule is a framework designed to facilitate a significant transformation in how healthcare data is managed, utilized, and shared across the sector. It emphasizes minimizing provider burden and advancing the interoperability framework, integrating Fast Healthcare Interoperability Resources (FHIR) APIs and SMART Applications into the healthcare IT ecosystem. This strategic alignment seeks to streamline healthcare operations, making the system more efficient, user-centric, and conducive to innovation. By laying down a foundation that promotes seamless data exchange and application integration, HTI-1 aims to catalyze the next wave of advancements in healthcare technology.
Certification Program Updates
A cornerstone of the HTI-1 Final Rule is its comprehensive overhaul of the certification program for healthcare IT. Moving away from the previous convention of year-themed editions, HTI-1 introduces a more dynamic and adaptable approach to certification. This shift entails the establishment of a single, unified set of certification criteria, termed “ONC Certification Criteria for Healthcare IT,” which simplifies the compliance process for developers and reduces the administrative overhead associated with updates. Moreover, it sets a precedent for a certification process that prioritizes clarity, efficiency, and relevance in the rapidly evolving landscape of healthcare technology.
- Discontinuation of Year-Themed “Editions”: Moving away from the previous convention, HTI-1 introduces a more dynamic certification approach, focusing on a unified set of criteria to streamline the update and compliance process.
- Single Set Certification: This novel approach consolidates certification criteria into a single set, simplifying the process for developers and reducing the need for comprehensive updates with each criterion change.
- Timely Utilization of Updates: Emphasizes the importance of swift adoption of updates by health IT developers, aiming to reduce confusion and align with industry advancements more effectively.
- Applicability and Expiration Timelines: Establishes clear timelines for the applicability and expiration of certification criteria, ensuring a structured and transparent approach to compliance.
Electronic Case Reporting (eCR) Enhancement
HTI-1 significantly advances electronic case reporting (eCR) with a focus on standardizing and improving the exchange of health data between healthcare providers and public health agencies. Key components include:
Requirement for Health IT Module Support:
- Mandate for Health IT Modules to support eCR using HL7 CDA and FHIR standards to standardize eCR data transmission.
- Aims to create a cohesive, interoperable environment that enhances data sharing and public health responsiveness.
Adoption Timeline for HL7 CDA or HL7 FHIR Implementation Guides:
- Developers are given until the end of 2024 to adopt HL7 CDA or HL7 FHIR implementation guides for eCR functionality.
- This phased implementation approach provides the necessary time for system alignment with standards.
Recommendations for Enhanced Connectivity:
- Recommendation 09: Real-world testing for Health IT Modules certified for either CDA or FHIR transmission of initial eCR data with a service to transform data into the non-implemented format, ensuring nationwide connectivity.
- Recommendation 10: Similar testing for modules certified only for CDA or FHIR exchange of Reportable Condition (RC) data, facilitating receipt of RC messages in either format by providers.
- Recommendation 11: Shift to real-world testing with “live” public health information systems or those specified by the public health community, improving system interconnectivity.
The Rationale for Recommendations
- Emphasizes the need for robust testing of system interconnectivity in the absence of a certification program for public health data systems.
- Aims to ensure well-tested, interoperable frameworks for eCR, addressing critical data handoff between providers and public health systems.
These steps underscore HTI-1’s commitment to enhancing public health surveillance and data exchange, streamlining the eCR process, and fostering a more interconnected health data ecosystem.
ONC Certification Criteria for Health IT and Discontinuing Year-Themed Editions
Background and Rationale:
- Moving away from year-themed editions to a unified certification approach.
- Aimed at simplifying the certification process and making it more adaptive to changes.
Proposed Approach:
- Introduction of “ONC Certification Criteria for Healthcare IT” as a single set for certification.
- Focus on specific updates without the need for complete re-certification, enhancing the process’s flexibility.
Benefits and Implications:
- Agility and Responsiveness: Enables health IT developers to swiftly adapt to new requirements and advancements.
- Reduced Burden: Simplifies updates, reducing the workload on developers and healthcare providers.
- Clarity and Transparency: Eliminates complexity, making the certification process more transparent.
User Impact:
- Ensures a smoother experience for users, facilitating easier updates and adaptation to new standards.
Industry Considerations:
- Emphasizes the importance of stakeholder feedback to balance the efficiency of the certification process with the stability and interoperability of healthcare IT systems
USCDI V3 Implementation
The United States Core Data for Interoperability version 3 (USCDI v3) represents an advanced set of standardized data elements and definitions, established to enhance healthcare data interoperability. It expands upon previous versions by introducing more comprehensive data elements that healthcare providers are expected to use for electronic health information exchange, aiming to improve patient care and public health outcomes through better data sharing and accessibility across different healthcare IT systems.
Transition Period for V1 and V3
The transition period given for the adoption of USCDI v1 to USCDI v3 extends until December 31, 2024. This timeframe allows healthcare IT developers and providers to adjust and update their systems to comply with the new version 3 standards. After the given date V3 will become the baseline.
Requirements for Health IT Module Updates
Modules must be updated to USCDI V3 by 2023, aligning with the US Core Implementation Guide and C-CDA companion guide for smooth integration.
Standardized API Revisions
Emphasis on adopting USCDI V3, US Core, and the SMART App launch framework for standardized APIs to boost interoperability.
Authentication and Authorization Standards:
It implements standards for authentication, authorization, and token introspection based on SMART version 2, ensuring secure data exchanges.
Publication API Maintenance
Calls for the revision and standardization of the service-based URL publication API, maintaining consistency and reliability in healthcare IT infrastructure.
The Shift to DSI (Decision Support Intervention)
Since 2012, ONC has been paving the way for a new standard known as the Decision Support Interventions (DSI) certification criterion to take over the existing CDS. The shift aligns with the evolving dynamics of healthcare decision-making, embracing advancements in functionalities, data elements, and software applications.
A Fresh Perspective on Decision Support
The transition from CDS to DSI represents more than just a name change. It signifies a strategic repositioning under the care coordination criteria, encapsulated in § 170.315(b). This enhancement broadens the scope of requirements, emphasizing the importance of source attributes and the configuration of both referential and evidence-based decision support interventions. A noteworthy addition is the inclusion of Health IT Modules that play a critical role in decision-making through predictive algorithms or models.
Enhancing Healthcare with Predictive Decision Support
The push towards DSI is fueled by the ambition to maximize the utility of predictive technologies in healthcare. The proposed changes are designed with four primary goals in mind:
- Improving Transparency: Shedding light on the design, development, training, and evaluation processes of predictive DSIs to bridge the knowledge gap in the market.
- Enhancing Trustworthiness: By ensuring transparency, the proposal aims to bolster confidence in how health IT developers manage and govern predictive DSIs.
- Supporting Consistency: The initiative seeks to standardize the availability of predictive DSI information, enabling users to comprehensively evaluate the technology’s quality and its adherence to fairness, appropriateness, validity, effectiveness, and safety standards (FAVES).
- Advancing Health Equity: The proposal addresses the urgent need to mitigate biases and health disparities exacerbated by predictive DSIs, advocating for their safe, appropriate, and equitable application.
Comprehensive Proposals for a Transformative Future
The HTI-1 proposed rule introduces several key proposals to realize these goals:
- Updated Source Attributes Requirements: An expansion in the number of source attributes and the variety of information available to users, especially concerning race, ethnicity, social determinants of health, and other critical data for health equity.
- Predictive DSI Requirements for Health IT Modules: A requirement for Health IT Modules to furnish additional information as source attributes, ensuring users can effectively assess and utilize predictive DSIs.
A Roadmap to Implementation
The proposed changes are accompanied by a clear timeline. By December 31, 2024, technologies currently certified under the CDS criterion must transition to the new DSI standard. This timeline also applies to meeting the Intervention Risk Management requirements. Furthermore, the Base EHR definition will evolve to include the revised DSI criterion exclusively starting January 1, 2025. In the interim, real-world testing of the technologies certified to either the existing CDS or the revised DSI criterion is mandated, ensuring a seamless and effective transition to the new era of decision support in healthcare.
The Complete List of Deadlines
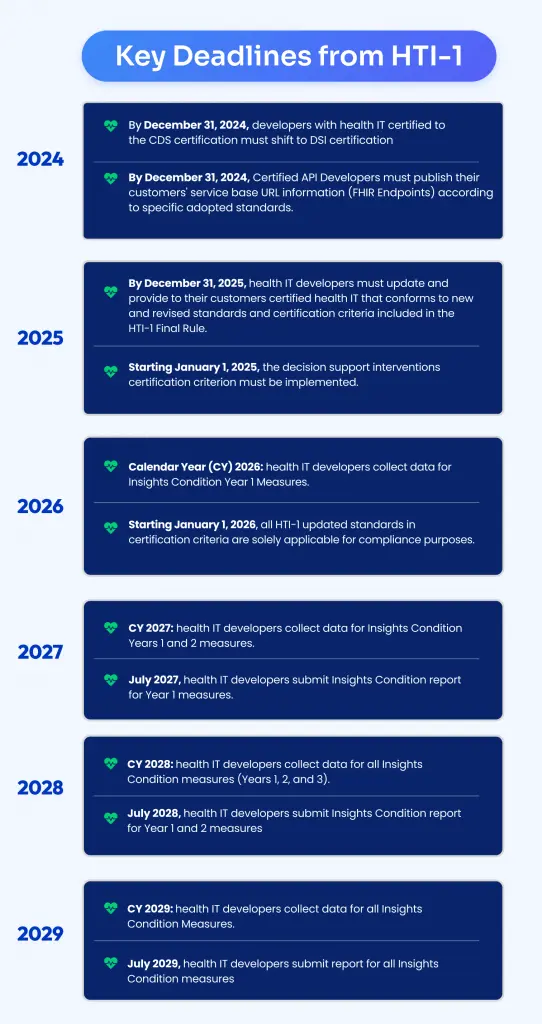
Overall Benefits of the HTI 1 Final Rule
This concise overview encapsulates the broader spectrum of benefits attributed to the rule, reflecting its impact on patients, healthcare providers, public health authorities, and health IT developers.
Enhancing Healthcare Delivery and Public Health
- Empowering Informed Decision-Making: Integrates advanced analytics for improved patient outcomes and equips providers with accurate, real-time information.
- Advancing Public Health: Empowers authorities with better data on disease outbreaks, facilitating timely and effective responses through enhanced data exchange.
Promoting Interoperability and Efficiency
- Enhancing Interoperability: Ensures seamless data exchange across systems, promoting standardization and reducing inconsistencies in implementation.
- Facilitating Efficient Updates: Aids in the swift adoption of new standards and features, ensuring that health IT systems remain current and compliant.
Fostering Collaboration and Compliance
- Encouraging Collaboration: Promotes partnerships between users and developers to customize new standards or functionalities, optimizing health IT integration.
- Supporting Regulatory Compliance: Aligns with other HHS programs like CMS’s Promoting Interoperability Program, ensuring timely updates to meet new or revised certification criteria.
Advancing Equity and User Experience
- Improving Health Equity: Addresses disparities by including diverse data attributes and focusing on equitable service delivery.
- Enhancing User Experience: Simplifies the health IT landscape for users, minimizing confusion and improving the usability of certified health IT.
Navigating Concerns and Recommendations Around HTI-1 Regulations
The introduction of the HTI 1 final rule by ONC has sparked a wide array of responses within the healthcare sector. While there is broad support for the regulation’s objectives, several concerns about its implementation and potential impact have emerged. This section outlines these apprehensions and suggests ways to mitigate them, ensuring the transition to HTI-1 is as smooth and beneficial as possible for all involved.
Addressing Implementation and Burden Concerns
- Implementation Timelines: A major concern lies in the aggressive timelines for implementing the extensive changes HTI-1 introduces. Stakeholders argue that these timelines may not provide adequate time for healthcare providers and IT developers to adapt, potentially leading to implementation challenges and disruptions.
- Provider and Developer Burden: There’s worry that the proposed rules might impose significant burdens on both healthcare providers and IT developers. The comprehensive nature of the HTI-1 changes demands considerable resources for adaptation and compliance, raising concerns about feasibility and the risk of operational strain.
Recommendations for a Smoother Transition
- Delayed Measurement Periods: To address concerns about readiness, it is recommended to delay the start of the first measurement period associated with the proposed Insights Condition to at least Calendar Year (CY) 2025. This delay would allow stakeholders more time to prepare, thus easing the transition.
- Extended Timeline for USCDI V3 Implementation: There’s a push to extend the implementation timeline for the USCDI Version 3 to the end of the second calendar year following the final rule’s publication, estimated to be December 31, 2025. This extension aims to give developers ample time for the necessary development and testing, facilitating smoother adoption.
Feedback on Specific Aspects of HTI-1
- ePA Requirements: The notable absence of electronic prior authorization (ePA) requirements in the HTI-1 proposals has been a point of disappointment for organizations such as America’s Health Insurance Plans (AHIP). AHIP underscores the benefits of ePA in streamlining care delivery, reducing administrative burdens, and cutting costs.
- Incremental Approach to ePA: Despite the concerns, there’s acknowledgment, notably from the Electronic Health Record Association (EHRA), of the government’s incremental steps towards integrating ePA. This cautious approach is seen as reflective of the complexity and scope of the proposed changes.
- Timing and Complexity Concerns: While there’s an appreciation for the thoughtful approach to rulemaking, vendors and industry experts express apprehension about the timing of introducing ePA requirements. The complex nature of the healthcare ecosystem necessitates a careful, consensus-driven standard development process to avoid unintended consequences.
Are We Moving Forward with HTI-1?
The feedback from various stakeholders underscores the need for a balanced and pragmatic approach to implementing the HTI-1 regulations. By considering the industry’s concerns and recommendations, there’s a pathway to achieving the regulations’ goals without overwhelming the healthcare system. This approach emphasizes the importance of collaboration, flexibility, and ongoing dialogue between healthcare providers, IT developers, and insurers to ensure that this transition supports the continued evolution and improvement of healthcare delivery.
We at Nalashaa have been helping HIT developers and Provider facilities solve their compliance challenges for over 13 years. With over 200k+ impacted clinics and 20+ HIT vendor certifications under our name, we can proudly say that compliance complexities don’t scare us. For a tailored solution to your needs connect with us.
Mitrajit Das
Latest posts by Mitrajit Das (see all)
- Revolutionizing Healthcare Communication: The AIDET Approach - March 17, 2025